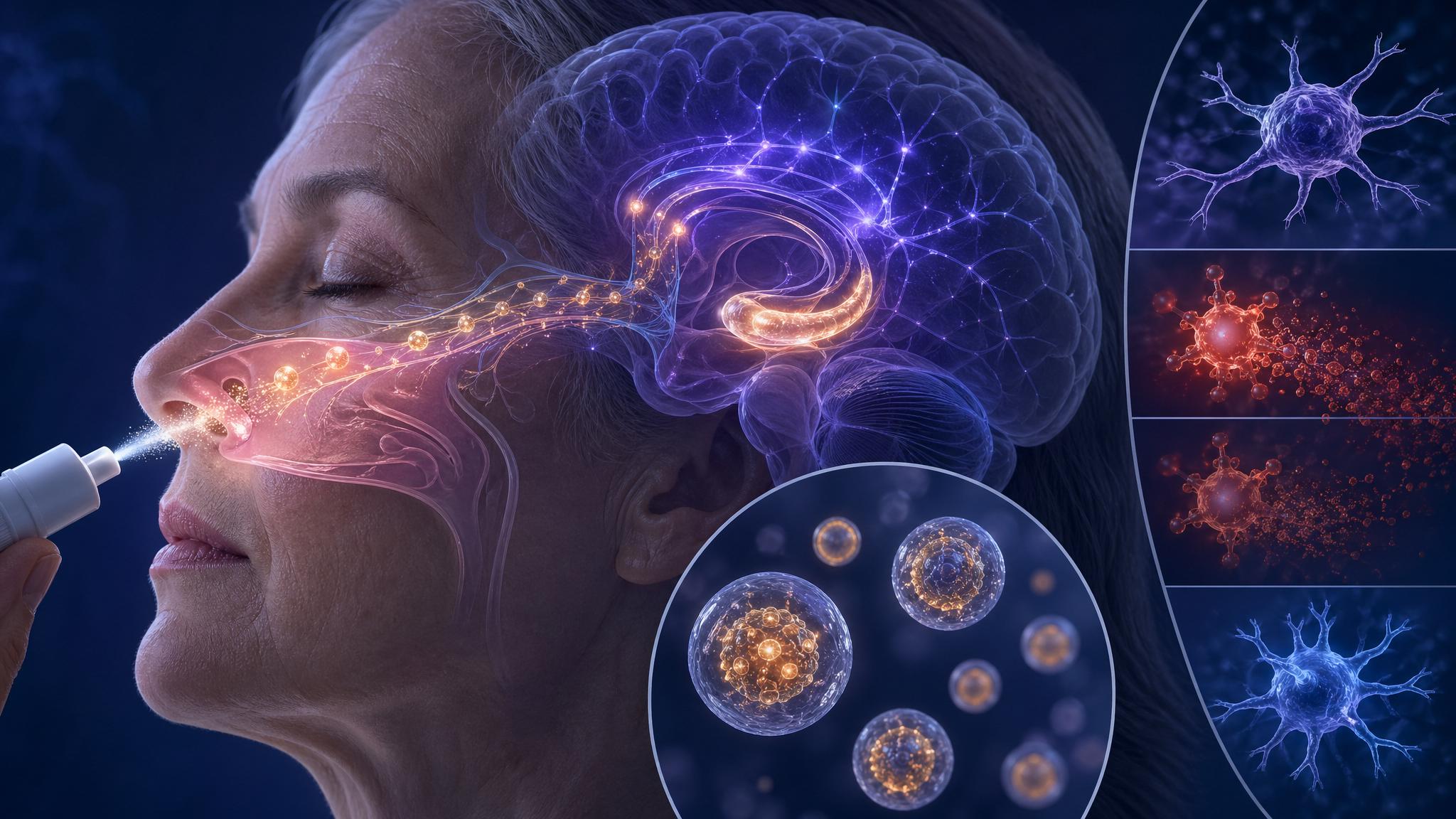
A Nasal Spray That Reverses Brain Aging: The Texas A&M Breakthrough Reshaping Alzheimer’s Research
A two-dose nasal spray built from human neural stem cell-derived particles silenced the inflammation signals that drive cognitive decline, restored memory in aged mice, and is now being positioned for human trials. Here is what the science reveals.
In April 2026, researchers at Texas A&M University published findings that may represent one of the most significant advances in brain aging science in years. Using a simple nasal spray loaded with microscopic particles derived from human neural stem cells, they reversed measurable markers of brain aging in aged mice, quieted the two most dangerous inflammatory signaling pathways in the aging brain, and restored memory performance that had declined with age. The effects lasted months after just two doses.
The study, published in the Journal of Extracellular Vesicles (15(2): e70232, 2026), was led by Dr. Ashok K. Shetty, a University Distinguished Professor and Associate Director of the Institute for Regenerative Medicine at the Texas A&M Naresh K. Vashisht College of Medicine, alongside senior research scientist Dr. Maheedhar Kodali and a team of collaborators including Leelavathi N. Madhu, Shama Rao, Sahithi Attaluri, Raghavendra Upadhya, and James J. Cai. The title states precisely what the team achieved: “Intranasal Human NSC-Derived EVs Therapy Can Restrain Inflammatory Microglial Transcriptome, and NLRP3 and cGAS-STING Signalling, in Aged Hippocampus.”
The implications reach far beyond a single mouse study. This research accelerates a platform approach to neurodegenerative disease that could eventually reshape how medicine delivers therapies directly to the brain.
The Aging Brain’s Silent Enemy: Neuroinflammation
To understand why this study matters, you first have to understand what happens to the brain as it ages. The process is not simply one of neurons dying off. It is a slow-burning inflammatory crisis driven by the brain’s own immune cells.
Microglia are the resident immune cells of the central nervous system. In a young, healthy brain, they perform surveillance duties: clearing cellular debris, pruning synapses, and responding to injury. But as the brain ages, microglia shift into a chronically activated state. They stop resolving inflammation and start perpetuating it. This condition, which researchers have begun calling “neuroinflammaging,” a fusion of neuroinflammation and aging, is now understood to be a primary driver of the cognitive decline that precedes Alzheimer’s disease, Parkinson’s disease, and other age-related dementias.
Alzheimer’s disease alone affects more than 6.9 million Americans, with global prevalence projected to nearly triple to 153 million by 2050, according to research published in The Lancet. The majority of people living with dementia will never be diagnosed until the disease is well advanced. That is because neuroinflammation damages the brain silently for years, often decades, before symptoms emerge.
The central challenge in targeting this inflammatory cascade has not been identifying the right pathways. Researchers have known for years which molecular systems drive chronic microglial activation. The challenge has been getting therapeutic agents past the blood-brain barrier, one of the most selective filters in human biology, to reach the specific brain regions that need intervention.
That is where the Texas A&M team made their pivotal contribution.
What Are Extracellular Vesicles?
Extracellular vesicles (EVs) are nanosized particles released naturally by cells throughout the body. They serve as biological messaging systems, carrying cargo of proteins, lipids, and nucleic acids from one cell to another. For decades they were dismissed as cellular waste products. The field’s rehabilitation has been swift: the 2016 Nobel Prize in Physiology or Medicine recognized autophagy, a related cellular housekeeping process, and since then the science of EVs has exploded.
What makes EVs remarkable for drug delivery is their stealth. Unlike synthetic nanoparticles, EVs are coated with biological membranes that the immune system recognizes as “self.” They evade immune clearance, travel through biological barriers with far greater efficiency than pharmaceutical compounds, and deliver their cargo with high specificity. When those EVs are derived from neural stem cells, they carry a payload that the brain’s own tissue is primed to receive.
The specific cargo in neural stem cell-derived EVs includes microRNAs: small, non-coding RNA molecules that do not encode proteins but instead regulate the expression of hundreds of target genes simultaneously. A single microRNA can modulate entire networks of inflammatory signaling. This is not a precision strike; it is a coordinated recalibration of the brain’s inflammatory state.
Dr. Shetty’s team derived their EVs from human neural stem cells, meaning the particles are biologically compatible with human tissue. They then packaged these EVs into a nasal spray formulation, targeting a delivery route that bypasses the blood-brain barrier entirely.
The Texas A&M Study: What the Researchers Found
The team tested their nasal spray on mice aged 18 months, the rodent equivalent of approximately a 60-year-old human. At this age, mouse brains display well-documented hallmarks of neuroinflammaging: elevated inflammatory cytokines, dysfunctional microglia, impaired hippocampal neurogenesis, and measurable deficits in learning and memory tasks.
The experimental animals received just two intranasal doses of the EV formulation. Within weeks, multiple converging lines of evidence pointed in the same direction.
Featured Partner
Invest in the Infrastructure Behind Modern Medicine
As healthcare expands beyond hospital walls, the buildings and campuses supporting that shift are generating compelling returns for investors who move early. The Healthcare Real Estate Fund offers qualified investors direct access to a curated portfolio of medical office, outpatient, and specialty care facilities.
Learn More →Inflammation markers in the hippocampus, the brain region most critical to memory formation and one of the earliest to show Alzheimer’s-related pathology, dropped measurably. The microglial transcriptome, the complete read-out of which genes the brain’s immune cells were expressing, shifted away from the pro-inflammatory activation profile characteristic of aged brains and toward a state more consistent with young, healthy tissue. Mitochondrial function in hippocampal cells improved, restoring the cellular energy supply that neurons need to maintain synaptic connections.
Performance on memory tests improved significantly. The animals treated with the nasal spray outperformed untreated age-matched controls on novel object recognition tasks, which measure the ability to detect new objects and notice changes in familiar environments. These cognitive improvements persisted for months after treatment.
Critically, the effects were sustained after just two doses. This is not a maintenance therapy requiring ongoing administration. It is a short-course intervention that appears to reset the brain’s inflammatory baseline and allow endogenous repair mechanisms to take over.
The NLRP3 Inflammasome and cGAS-STING: The Twin Drivers
Two molecular systems sit at the center of this research: the NLRP3 inflammasome and the cGAS-STING signaling pathway. Understanding what they do helps explain why suppressing them has such a powerful effect on brain aging.
The NLRP3 inflammasome is a multi-protein complex inside immune cells that acts as a sentinel for cellular danger signals. When it detects oxidative stress, mitochondrial dysfunction, or accumulated cellular debris, all of which increase with age, it assembles and triggers the release of interleukin-1 beta and interleukin-18, two of the most potent pro-inflammatory cytokines in the body. In the young brain, NLRP3 activation is transient and self-limiting. In the aging brain, it becomes constitutively active, generating a low-grade inflammatory signal that slowly degrades neural circuitry.
The cGAS-STING pathway operates on a different trigger. cGAS, cyclic GMP-AMP synthase, acts as a sensor for cytosolic DNA: specifically, DNA that should not be freely floating inside cells. As cells age, their mitochondria become leaky, releasing mitochondrial DNA into the cytoplasm. cGAS detects this mislocalized DNA, activates STING (stimulator of interferon genes), and launches an interferon-mediated inflammatory response. Recent research published in Nature Reviews Neuroscience has identified hyperactivated cGAS-STING signaling as a consistent feature of the aging brain and a likely contributor to the neuroinflammatory milieu that precedes Alzheimer’s pathology.
The EV-delivered microRNAs in the Texas A&M formulation suppressed both of these systems simultaneously. This is important because NLRP3 and cGAS-STING operate through partially independent mechanisms. A therapy that only blocks one pathway may find the other compensating for it. By recalibrating the microglial transcriptome broadly, rather than targeting a single inflammatory mediator, the EV approach achieves a more durable resolution of the inflammatory state.
How the Nasal Route Changes Everything
One of the most important aspects of this research is not what the therapy does inside the brain but how it gets there.
The blood-brain barrier is an extraordinarily selective filter made up of tightly joined endothelial cells lining the brain’s blood vessels. It keeps pathogens, large molecules, and most pharmaceutical compounds out of the central nervous system. This protective function is also one of the primary reasons that approximately 98 percent of small-molecule drugs and nearly all large-molecule biologics cannot reach the brain in therapeutic concentrations.
Conventional approaches to bypassing the barrier have included direct surgical injection into brain tissue, intrathecal delivery via lumbar puncture, and focused ultrasound to temporarily open the barrier. All of these methods carry risks that limit their use to patients with established disease who have no other options.
The nasal route offers a fundamentally different alternative. When particles are administered intranasally, a subset of them can travel along the olfactory and trigeminal nerves, which project directly from the nasal mucosa into brain tissue, bypassing the barrier entirely. This pathway has been studied for several decades in the context of insulin delivery and neuropeptide administration. The Texas A&M team exploited this route to deliver their EV cargo directly to hippocampal tissue with no surgical intervention and no systemic exposure.
The delivery format itself, a nasal spray, is one of the most patient-friendly administration routes in medicine. It requires no injection, no hospitalization, and no specialized clinical infrastructure. If the approach translates to humans, it could enable preventive neurology at a population scale that is simply not achievable with infusions or surgical procedures.
From Mouse to Human: The Road Ahead
The researchers are careful to note that human trials for this nasal spray are still years away. Extensive preclinical safety testing is needed to characterize the biodistribution of the EV formulation, establish dose-response relationships across a broader age range, confirm that the immunological profile of human neural stem cell-derived EVs is acceptable for repeated clinical use, and rule out off-target effects in non-brain tissue.
Manufacturing scale is also a consideration. Producing clinical-grade extracellular vesicles from human neural stem cells requires quality-controlled cell lines, validated isolation and purification protocols, and rigorous potency assays. The field is advancing rapidly on all of these fronts. Several biotech companies, including Evox Therapeutics, Codiak BioSciences (prior to its restructuring), and Anjarium Biosciences, have developed GMP-compatible EV manufacturing platforms that could in principle be adapted for this type of neural stem cell-derived product.
The broader scientific trajectory is encouraging. This is not an isolated finding. A 2024 paper from Madhu et al. in the Journal of Extracellular Vesicles demonstrated that hiPSC-derived neural stem cell EVs could reduce amyloid-beta plaques and phosphorylated tau in Alzheimer’s disease models when administered early in disease progression. The 2026 Texas A&M study builds on that prior work and extends it into the context of normal aging, a much larger potential target population that includes every adult over the age of 50.
The fact that the study used mice aged at a point equivalent to early-to-middle human senescence is particularly meaningful. Most Alzheimer’s research focuses on late-stage disease models where pathology is already established. Demonstrating efficacy in a model of early neuroinflammaging suggests that this approach could work as a preventive or very early-stage intervention, precisely the window where it would have the greatest impact on disease trajectory.
The Bigger Picture: Extracellular Vesicles as a Platform
What makes the Texas A&M approach scientifically important beyond its Alzheimer’s implications is the broader principle it validates: that biological nanoparticles derived from stem cells can serve as programmable delivery vehicles for CNS therapeutics.
The microRNA cargo inside these EVs can, in principle, be modified. Different microRNA combinations target different pathways. A formulation optimized for Alzheimer’s prevention might emphasize NLRP3 and cGAS-STING suppression, as in this study. A formulation designed for Parkinson’s disease might instead prioritize alpha-synuclein clearance pathways and lysosomal function. A post-traumatic brain injury application might focus on acute neuroinflammation resolution. The delivery vehicle is the same; the cargo is customized.
This platform logic is exactly the kind of “biological coordination” framework that researchers at the 2nd World Congress on Targeting Longevity, held in Berlin earlier this month, argued was necessary to move beyond single-target interventions in aging science. The cGAS-STING findings intersect directly with senescence biology, where accumulated senescent cells release a senescence-associated secretory phenotype (SASP) that includes cGAS-STING activators. Therapies that suppress this signaling cascade may therefore simultaneously address neuroinflammation and the cellular senescence burden that accumulates with age.
Viewed through this systems lens, the Texas A&M nasal spray is not simply a delivery mechanism for anti-inflammatory microRNAs. It is a first clinical prototype for programmable biological coordination of the aging brain.
What This Means for You
The honest answer is that this specific nasal spray is not available and will not be for several years at minimum. Human trials have not yet begun, and translating mouse findings into safe, effective human therapies is a long and uncertain process. Nothing about this research should change your medication regimen or clinical decisions without your physician’s involvement.
What it does change is the landscape of possibility. For the first time, there is strong preclinical evidence that the NLRP3 and cGAS-STING inflammatory cascades in the aging hippocampus can be durably suppressed with a non-invasive, low-dose biological intervention. That is a meaningful shift in where the science stands.
In the meantime, the same neuroinflammatory pathways that this nasal spray suppresses are directly modulated by lifestyle factors that are available to you today. Resistance and aerobic exercise have both been shown to reduce NLRP3 inflammasome activation and improve microglial homeostasis, with VO2 max strongly predicting hippocampal volume preservation into older age. Sleep, specifically the deep slow-wave stages that consolidate memory and clear metabolic waste via the glymphatic system, is one of the most powerful regulators of microglial activation state. Diets high in polyphenols, omega-3 fatty acids, and fermented foods modulate the gut-brain axis in ways that reduce systemic inflammatory signals reaching the brain. Chronic psychological stress activates cGAS-STING through mitochondrial damage, which is one of the many reasons that breathwork, meditation, and stress regulation are not peripheral wellness practices but core neuroprotective strategies.
If the Texas A&M nasal spray enters human trials in the next few years, the patients most likely to benefit from it will be those who arrive at the clinic with the lowest baseline neuroinflammatory burden. In other words, the foundational practices you build today are not a substitute for the coming pharmacological breakthroughs in brain aging. They are the preparation that will make those breakthroughs matter more when they arrive.
The thread of longevity is being rewoven, one study at a time.
Sources: Shetty AK et al., Journal of Extracellular Vesicles, 15(2): e70232, 2026. Texas A&M Institute for Regenerative Medicine press release, April 14, 2026. Madhu LN et al., Journal of Extracellular Vesicles, 2024. Alzheimer’s Disease International World Alzheimer Report. Nature Reviews Neuroscience, cGAS-STING in neurodegeneration, 2024 to 2025.